-
×
 Coral Calcium
1 × $30.99
Coral Calcium
1 × $30.99 -
×
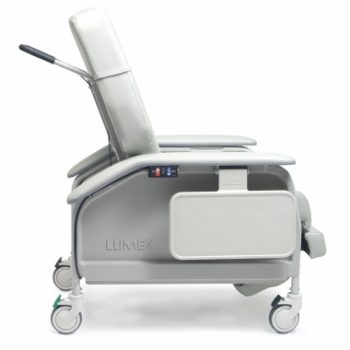 Recl Xwd Heat&Mas Port Ca-133, Lumex
1 × $3,732.00
Recl Xwd Heat&Mas Port Ca-133, Lumex
1 × $3,732.00 -
×
 Bed Pkg Se Roll Foam Fr Pl End Lumex
1 × $1,134.00
Bed Pkg Se Roll Foam Fr Pl End Lumex
1 × $1,134.00 -
×
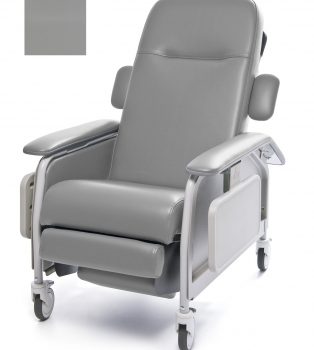 Recliner Cl Care Dove Ca133 Lumex
1 × $2,068.00
Recliner Cl Care Dove Ca133 Lumex
1 × $2,068.00 -
×
 Thermometer Flt Bath Frnt/Cent Grafco
1 × $13.92
Thermometer Flt Bath Frnt/Cent Grafco
1 × $13.92 -
×
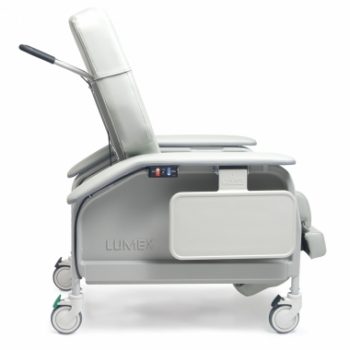 Recl Xwd Heat&Mas Eucalyptus Ca-133, Lumex
1 × $3,732.00
Recl Xwd Heat&Mas Eucalyptus Ca-133, Lumex
1 × $3,732.00 -
×
 Trach Jcksn Shrt Stnls Stl #5 John Bunn
1 × $136.54
Trach Jcksn Shrt Stnls Stl #5 John Bunn
1 × $136.54 -
×
 Sling Cradle Arm Universal Sz Grafco
1 × $10.80
Sling Cradle Arm Universal Sz Grafco
1 × $10.80 -
×
 #Sphyg Labstar Thigh (Blk) Latex Free, Labtron
1 × $33.58
#Sphyg Labstar Thigh (Blk) Latex Free, Labtron
1 × $33.58 -
×
 W/C Trans Chair Pink Alum 19 E&J
1 × $228.00
W/C Trans Chair Pink Alum 19 E&J
1 × $228.00 -
×
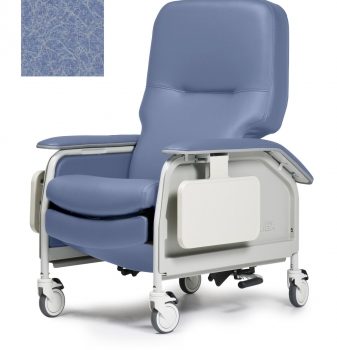 Recliner Dlx Cl Care Ice Blue Ca133 Lumex
1 × $2,290.00
Recliner Dlx Cl Care Ice Blue Ca133 Lumex
1 × $2,290.00 -
×
 W/C Advant Rcl 18X17 Full Elr Notify Cust Of High Freight
1 × $530.00
W/C Advant Rcl 18X17 Full Elr Notify Cust Of High Freight
1 × $530.00 -
×
 Alpha (R) CF
1 × $11.49
Alpha (R) CF
1 × $11.49 -
×
 W/C Trans Bariatric Chair 24W Al E&J **On Temporary Hold**
1 × $440.00
W/C Trans Bariatric Chair 24W Al E&J **On Temporary Hold**
1 × $440.00 -
×
 W/C Trans Chair Blue Alum 19 E&J
1 × $228.00
W/C Trans Chair Blue Alum 19 E&J
1 × $228.00 -
×
 W/C Trans Silver Vein Steel 19 E&J
1 × $184.00
W/C Trans Silver Vein Steel 19 E&J
1 × $184.00 -
×
 Iv Pole Wheelchair 1-Hook Lumex
1 × $80.50
Iv Pole Wheelchair 1-Hook Lumex
1 × $80.50 -
×
 Nipper Nail 4-1/2" Grafco
1 × $30.52
Nipper Nail 4-1/2" Grafco
1 × $30.52 -
×
 W/C Htc 22X18 Desk Elr E&J
1 × $550.00
W/C Htc 22X18 Desk Elr E&J
1 × $550.00 -
×
 W/C Trans Chair Green Alum 17" E&J
1 × $228.00
W/C Trans Chair Green Alum 17" E&J
1 × $228.00 -
×
 W/C Rsc Ss Hi-Bk Pin Lk E&J
1 × $1,382.00
W/C Rsc Ss Hi-Bk Pin Lk E&J
1 × $1,382.00 -
×
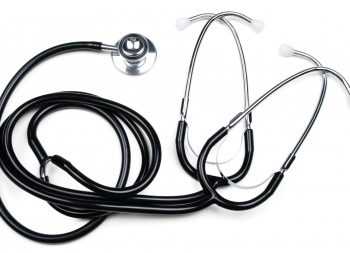 #Teaching Dual Steth Lot#
1 × $16.38
#Teaching Dual Steth Lot#
1 × $16.38 -
×
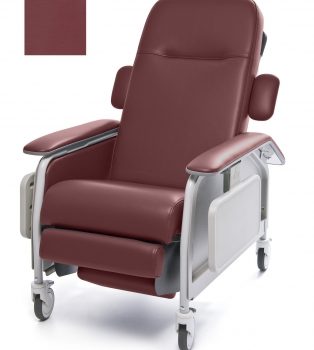 Recliner Cl Care Port Ca133 Lumex
1 × $2,068.00
Recliner Cl Care Port Ca133 Lumex
1 × $2,068.00 -
×
 Recl Heat&Mas Steel Blue Ca-133, Lumex
1 × $3,130.00
Recl Heat&Mas Steel Blue Ca-133, Lumex
1 × $3,130.00 -
×
 #Dark Blue Sprague Stethoscope Lot #
1 × $18.44
#Dark Blue Sprague Stethoscope Lot #
1 × $18.44 -
×
 First Aid Kit Pltic-10 Person Grafco
1 × $27.48
First Aid Kit Pltic-10 Person Grafco
1 × $27.48 -
×
 Cat's Claw Bark
1 × $11.49
Cat's Claw Bark
1 × $11.49 -
×
 Chair Pressure Pad For P Alarm Lumex
1 × $47.00
Chair Pressure Pad For P Alarm Lumex
1 × $47.00 -
×
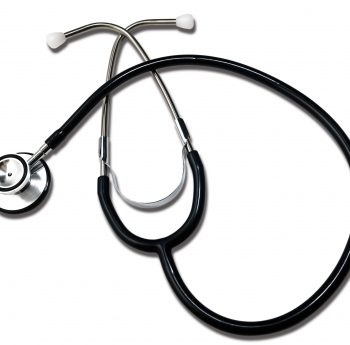 Steth Dual Head Blk Labtron
1 × $6.90
Steth Dual Head Blk Labtron
1 × $6.90 -
×
 Arnica montana 30X
1 × $9.99
Arnica montana 30X
1 × $9.99 -
×
 Comfort Cushion 16X16X3 E&J
1 × $34.00
Comfort Cushion 16X16X3 E&J
1 × $34.00 -
×
 Vitamin C 500 mg with Bioflavonoids
1 × $10.49
Vitamin C 500 mg with Bioflavonoids
1 × $10.49 -
×
 Zinc Chelate
1 × $7.49
Zinc Chelate
1 × $7.49 -
×
 Vitamin D3 5,000 IU
1 × $18.99
Vitamin D3 5,000 IU
1 × $18.99 -
×
 Vitamin B2
1 × $8.49
Vitamin B2
1 × $8.49 -
×
 Yarrow Flowers
2 × $5.99
Yarrow Flowers
2 × $5.99 -
×
 Vitamin D3 2,000 IU
1 × $8.99
Vitamin D3 2,000 IU
1 × $8.99 -
×
 Willow
1 × $9.99
Willow
1 × $9.99 -
×
 White Oak Bark
1 × $9.49
White Oak Bark
1 × $9.49
Subtotal: $22,529.93

